A skin rash is a noticeable change in the texture, color, or appearance of your skin. It can appear as red patches, bumps, blisters, dryness, or even peeling. Rashes are extremely common – almost everyone experiences at least one during their lifetime. They may be localized to one area or spread across large parts of the body.
While most rashes are harmless and resolve on their own, some can signal an underlying medical condition that requires attention. This comprehensive guide covers everything you need to know about skin rashes: causes, types, symptoms, home remedies, medical treatments, prevention, and when to worry.
What Is a Skin Rash?
A skin rash is any area of irritated, inflamed, or swollen skin. It often differs from surrounding skin in color, texture, or temperature. Rashes can be flat, raised, bumpy, scaly, or blistered. They may cause itching, burning, stinging, or pain. Some rashes appear suddenly, while others develop gradually. The duration can range from a few hours to several weeks, depending on the cause.
Allergic Reactions and Skin Rash
One of the most common triggers is an allergic reaction. When your immune system overreacts to a normally harmless substance (allergen), it releases histamines that cause blood vessels to leak fluid into the skincare, leading to redness, swelling, and itching. Common allergens include certain foods (nuts, shellfish, eggs), medications (penicillin, aspirin), insect stings, latex, or pet dander. Allergic rashes often appear as hives – raised, red, itchy welts that can change shape and move around the body.
Common Causes of Skin Rash
Skin rashes arise from a wide variety of triggers. Below are the most frequent causes:
- Allergens – Pollen, dust mites, mold, animal dander, certain foods, or medications.
- Irritants – Soaps, detergents, cosmetics, perfumes, chemicals, or fabrics (wool, polyester).
- Infections – Viral (chickenpox, measles, shingles), bacterial (impetigo, scarlet fever), fungal (ringworm, yeast), or parasitic (scabies, lice).
- Heat and sweat – Blocked sweat ducts cause heat rash, especially in hot, humid weather.
- Autoimmune conditions – Psoriasis, lupus, or dermatomyositis.
- Stress – Emotional stress can trigger or worsen rashes like eczema or hives.
- Environmental factors – Sun exposure (sun rash), cold weather (chapped skin), or dry air.
Heat Rash and Its Causes
Heat rash (miliaria) occurs when sweat ducts become blocked and sweat leaks into the surrounding skin. It is very common in hot, humid climates or after intense physical activity. Babies are especially prone because their sweat ducts are not fully developed. Heat rash appears as tiny red or clear bumps, often on the neck, chest, groin, or armpits. It usually clears up once the skin cools down.
Contact Dermatitis Explained
Contact dermatitis is a localized rash caused by direct contact with an irritant or allergen. There are two types:
- Irritant contact dermatitis – More common, caused by harsh chemicals like bleach, battery acid, or repeated handwashing. It burns or stings more than it itches.
- Allergic contact dermatitis – An immune reaction to substances like poison ivy, nickel (in jewelry), fragrances, or preservatives. It often appears 24–48 hours after exposure.
The rash is typically red, itchy, and may blister or ooze. Avoiding the trigger is the main treatment.
Viral and Bacterial Skin Rashes
- Viral rashes – Many viral infections cause skin rashes. Examples: measles (flat red spots that start on the face), chickenpox (itchy blisters), shingles (painful band of blisters), and hand-foot-and-mouth disease (small red spots on palms, soles, and mouth). Viral rashes often come with fever, cough, or fatigue.
- Bacterial rashes – Scarlet fever (fine red rash like sandpaper), impetigo (honey‑colored crusty sores), and cellulitis (red, swollen, tender area that spreads). Bacterial rashes usually require antibiotics.
Types of Skin Rash You Should Know
Not all rashes look the same. Recognizing the type can help identify the cause:
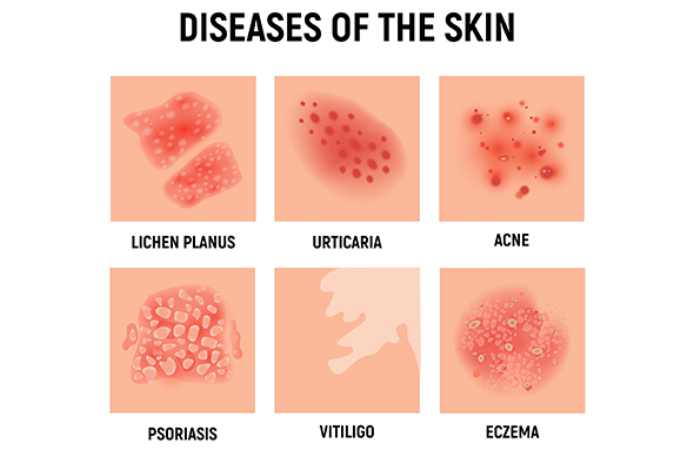
- Eczema (atopic dermatitis) – Dry, scaly, intensely itchy patches, often on the face, elbows, and knees. Common in children with allergies or asthma.
- Psoriasis – Thick, red patches covered with silvery scales, usually on the scalp, elbows, knees, and lower back. It is an autoimmune condition.
- Hives (urticaria) – Raised, red, itchy welts that appear suddenly and fade within hours. Often due to allergies or stress.
- Heat rash – Small, red or clear bumps in sweaty areas (neck, chest, groin).
- Ringworm (tinea) – Circular, red, scaly patches with a clear center, resembling a ring. It is a fungal infection.
- Intertrigo – Red, raw rash in skin folds (under breasts, belly, armpits) caused by friction and moisture.
- Rosacea – Facial redness with visible blood vessels and sometimes pimple‑like bumps.
- Lichen planus – Purplish, flat, itchy bumps on the wrists, ankles, or inside the mouth.
Symptoms of Skin Rash
Symptoms vary depending on the cause, but most rashes share common features.
Itching, Redness, and Swelling Symptoms
- Itching (pruritus) – The most common symptom. It can be mild to severe and may worsen at night.
- Redness (erythema) – Caused by increased blood flow to the affected area.
- Swelling (edema) – Fluid accumulation in the skin, making it feel tight or puffy.
- Blisters or vesicles – Small fluid‑filled bumps.
- Dry, cracked, or scaly skin – Often seen in eczema or fungal infections.
- Pain or burning – More typical in irritant contact dermatitis or shingles.
- Oozing or crusting – Indicates infection or weeping eczema.
Additional systemic symptoms (fever, chills, joint pain, swollen lymph nodes) suggest an underlying infection or autoimmune disease.
When to See a Doctor for Skin Rash
Most rashes are not emergencies, but certain signs warrant professional medical attention.
When Skin Rash Becomes Dangerous
Seek immediate medical care if you experience:
- Sudden, rapidly spreading rash – Especially if accompanied by fever or difficulty breathing.
- Blisters in the mouth, eyes, or genitals – Could be Stevens‑Johnson syndrome (a severe drug reaction).
- Rash that looks like a target or bullseye – Possibly Lyme disease from a tick bite.
- Painful, red, swollen, and warm rash – May indicate cellulitis (bacterial skin infection) that can spread to the bloodstream.
- Rash with high fever – Could be meningitis, measles, or toxic shock syndrome.
- Rash that does not fade when pressed (non‑blanching) – Use a glass test: press a clear glass against the rash. If it remains red/purple, it may be vasculitis or meningococcal disease.
Also see a doctor if:
- The rash covers a large portion of your body.
- Home remedies do not improve it after a few days.
- It is extremely painful or keeps you awake.
- You have a weakened immune system (cancer, HIV, transplant).
Home Remedies for Skin Rash Relief
Many mild rashes can be managed at home with simple, natural remedies.
Best Natural Remedies for Skin Rash
- Cool compress – Apply a clean cloth soaked in cool water for 15–20 minutes several times a day. Reduces itching and swelling.
- Oatmeal bath – Add colloidal oatmeal (finely ground oats) to lukewarm bath water. Soothes eczema, poison ivy, and chickenpox.
- Aloe vera – Apply pure aloe vera gel from the plant. Calms sunburn and minor irritations.
- Coconut oil – Virgin coconut oil moisturizes dry, itchy skin and has mild antibacterial properties.
- Baking soda paste – Mix 3 parts baking soda with 1 part water. Apply to insect bites or poison ivy for 10 minutes.
- Apple cider vinegar – Dilute with equal parts water and dab on fungal rashes (ringworm). Do not use on broken skin.
- Chamomile or calendula tea compress – Steep tea bags, cool them, and press on the rash.
Over-the-Counter Treatments for Relief
For fast relief without a prescription:
- Hydrocortisone cream (1%) – Reduces inflammation and itching. Use for eczema, insect bites, or contact dermatitis. Do not use on fungal or viral rashes.
- Antihistamines – Oral options like diphenhydramine (Benadryl) or cetirizine (Zyrtec) relieve allergic rashes and hives.
- Calamine lotion – Soothes poison ivy, chickenpox, and mild heat rash.
- Topical anesthetics – Products with pramoxine or lidocaine numb the area temporarily.
- Moisturizers (emollients) – Fragrance‑free creams with ceramides or petrolatum restore the skin barrier.
- Antifungal creams – Clotrimazole or miconazole for ringworm, athlete’s foot, or yeast rashes.
- Antibiotic ointment – Bacitracin or Neosporin only for minor infected cuts, not for general rashes.
Medical Treatments for Skin Rash
If home care fails, a doctor may prescribe stronger treatments:
- Prescription corticosteroids – Stronger hydrocortisone (e.g., triamcinolone cream) or oral prednisone for severe inflammation.
- Antibiotics – Oral or topical for bacterial infections (impetigo, cellulitis).
- Antiviral drugs – Acyclovir or valacyclovir for shingles or herpes.
- Antifungal pills – Terbinafine or fluconazole for widespread fungal infections.
- Immunomodulators – Tacrolimus or pimecrolimus for eczema unresponsive to steroids.
- Biologics – Injectable drugs (e.g., dupilumab) for severe atopic dermatitis or psoriasis.
- Phototherapy – Controlled UV light exposure for psoriasis and eczema.
Always follow the doctor’s instructions. Do not share prescription medications.
How to Prevent Skin Rash
Prevention is often easier than treatment. Adopt these habits.
Tips to Avoid Skin Irritation
- Identify and avoid triggers – Keep a diary to track what you ate, used, or touched before a rash appeared.
- Use gentle, fragrance‑free products – Soaps, detergents, lotions, and cosmetics labeled “hypoallergenic” or “for sensitive skin”.
- Moisturize daily – Apply a thick, fragrance‑free moisturizer right after bathing to lock in moisture.
- Wear loose, breathable fabrics – Cotton and bamboo are best. Avoid wool, nylon, and tight clothing.
- Stay cool and dry – Shower after sweating, change out of wet clothes, and use fans or air conditioning in hot weather.
- Test new products – Do a patch test on a small area of skin (e.g., inner forearm) for 3–5 days before full use.
- Manage stress – Stress triggers or worsens many rashes. Practice relaxation techniques, exercise, and adequate sleep.
- Protect your skin from the sun – Use broad‑spectrum sunscreen (SPF 30+). Some rashes (like lupus or polymorphous light eruption) are sun‑induced.
- Avoid known allergens – If you have food allergies, read labels carefully. For pollen allergies, keep windows closed and shower after being outdoors.
Skin Rash in Children vs Adults
Rashes can present differently across age groups.
- Children are more likely to have viral rashes (measles, chickenpox, fifth disease), heat rash, diaper rash, and eczema. Their immune systems are still developing. Many childhood rashes come with fever. Always consult a pediatrician before giving any medication.
- Adults – More prone to contact dermatitis from work or hobbies, shingles (due to previous chickenpox virus reactivation), psoriasis, and medication‑induced rashes. Chronic conditions like diabetes or kidney disease can also cause rashes.
Key difference: Children often outgrow eczema, while adults may develop new allergies over time. A rash in an adult that persists or recurs should be evaluated for underlying systemic disease.
Is Skin Rash a Sign of a Serious Condition?
Most rashes are benign, but sometimes they signal a serious health problem.
Rashes that can indicate serious conditions:
- Meningitis – Non‑blanching rash (does not fade under pressure) with fever, stiff neck, and headache. Medical emergency.
- Lyme disease – Bullseye rash (erythema migrans) after a tick bite. Can lead to arthritis, heart problems, and neurological issues if untreated.
- Toxic shock syndrome – Sunburn‑like rash with high fever, vomiting, and low blood pressure. Linked to tampon use or surgical wounds.
- Stevens‑Johnson syndrome / Toxic epidermal necrolysis – Painful red rash that blisters and causes skin to peel off in sheets. Usually a drug reaction. Life‑threatening.
- Autoimmune diseases – Lupus (butterfly rash on face), dermatomyositis (purple rash on eyelids and knuckles), or vasculitis (purple spots).
- Cancer – Rarely, itchy rashes can be a sign of lymphoma (mycosis fungoides) or internal malignancy (paraneoplastic rash).
Bottom line: If a rash comes with systemic symptoms (fever, weight loss, night sweats, joint pain, or fatigue) or does not respond to basic care, see a doctor promptly.
Conclusion
Skin rashes are an incredibly common yet diverse group of conditions. Understanding the cause – whether allergic, infectious, irritant, or autoimmune – is the first step to effective relief. Most rashes are mild and can be managed with home remedies like cool compresses, oatmeal baths, and over‑the‑counter creams.
However, knowing the red flags (non‑blanching rash, high fever, rapid spreading, blisters in sensitive areas) can save lives by prompting timely medical intervention.
Prevention through gentle skin care, trigger avoidance, and stress management is your best long‑term strategy. Children and adults may experience different types of rashes, but the principles of treatment and when to worry remain similar.
Frequently Asked Questions
Q1: How long does a typical skin rash last?
It depends on the cause. Heat rash often clears in 2–3 days. Allergic contact dermatitis may take 2–4 weeks. Viral rashes usually fade within 5–14 days. Chronic conditions like eczema or psoriasis can last months or years.
Q2: Can stress cause a skin rash?
Yes. Emotional stress triggers the release of cortisol and other hormones that can worsen eczema, hives, psoriasis, and rosacea. Stress management techniques often help reduce flare‑ups.
Q3: Is a rash contagious?
Only if the cause is infectious. Viral rashes (chickenpox, measles), bacterial rashes (impetigo, scarlet fever), fungal rashes (ringworm), and parasitic rashes (scabies) are contagious. Allergic and autoimmune rashes are not.
Q4: What is the fastest way to stop itching from a rash?
A cool compress or an over‑the‑counter oral antihistamine (like cetirizine) provides rapid relief. Avoid hot showers and scratching, which make itching worse.
Q5: Should I use an antibiotic cream on every rash?
No. Antibiotic creams only work on bacterial infections. They can actually irritate allergic or fungal rashes. Use only if your doctor confirms a bacterial cause.
Q6: Can food allergies cause a skin rash without other symptoms?
Yes. Some people develop hives or eczema from food allergens without digestive or respiratory symptoms. Common triggers include nuts, milk, eggs, soy, wheat, and shellfish.
Q7: When is a rash an emergency?
Go to the ER immediately if the rash appears suddenly along with difficulty breathing, swelling of the face or throat, high fever, confusion, or if it does not fade when pressed (non‑blanching).
Q8: Can I shower with a rash?
Yes, but use lukewarm water (not hot) and a mild, fragrance‑free cleanser. Pat dry – do not rub. Apply moisturizer immediately after.
Q9: Why does my rash only appear at night?
Itching often worsens at night due to natural cortisol dips and lack of distraction. Also, some causes, like scabies mites, are more active in the evening. Bedding allergens (dust mites) may also play a role.
Q10: Are natural remedies always safe?
Not always. Essential oils (tea tree, lavender) can cause allergic contact dermatitis. Lemon juice can cause phytophotodermatitis (severe sunburn). Always do a patch test and dilute as directed.

